Essentials
- Your body can take time to heal itself.
- Symptoms continuing for more than 6 months are known as Post Treatment Lyme Disease Syndrome (PTLDS).
- The cause of some cases of post treatment Lyme arthritis has been found.
- The cause of most PTLDS in Europe is unknown.
- It is currently thought that in some cases Lyme disease may alter the immune system, causing lasting symptoms.
- Research to find the cause and treatment of PTLDS is continuing.
What are the possible causes of continuing symptoms?
- Your body needs time. If Lyme disease has given you pain, the communications in your nervous system and immune system may have been upset. This can result in messages of pain still being sent to your brain, even though the cause (Lyme disease) has been dealt with. It can take time for your system to re-set itself and get back to normal. The best way to cope with this is to live as normally as you can – be active and positive to help teach your body to re-set. Persistent pain can be caused by many injuries – not just Lyme disease. Read more about persistent pain on the NHS Cumbria website.
- Continuing active infection. Most researchers think it is unlikely that the bacteria survive antibiotics, but it is possible [1]. It is, however, difficult to prove bacteria are still present without analysing samples of body tissue with a PCR test for the Borrelia bacteria. Sometimes a repeat course of treatment with a different antibiotic has provided a cure. [2]
- Post Antibiotic Lyme Arthritis. There are cases of definite Lyme Arthritis (diagnosed by a positive PCR of joint fluid) when the joint swelling has continued after treatment. A negative PCR on joint fluid implies that the Borrelia bacteria have been killed by the antibiotics. Treatment with Disease Modifying Anti Rheumatic Drugs resolves the symptoms. [3] Lyme Arthritis is rare in Europe.
- Tissue damage. Some symptoms, especially those due to nerve damage, like a facial palsy, can take a long time to gradually resolve.
- Post Treatment Lyme Disease Syndrome. See the discussion of this below. At the moment the cause and treatment of this is unknown.
Post Treatment Lyme Disease Syndrome
Although some people take many weeks to recover after treatment, particularly the elderly [9], it has now been recognised that continuing symptoms can go on for longer, This is now termed Post Treatment Lyme Disease Syndrome (PTLDS) [4] and has the following definition:
Onset of fatigue, widespread pain or cognitive difficulties (sometimes called brain fog) within 6 months of completing appropriate antibiotic treatment.
See the full definition in the table below reproduced from the paper 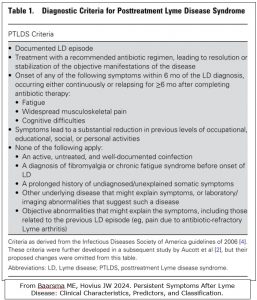
Note that this definition is based on American Lyme disease and may not be appropriate for European Lyme disease, but it is the only definition agreed by doctors and researchers at the moment.
What causes PTLDS?
No one knows at the moment. Most European research on Lyme disease has been conducted on relatively early diagnosed patients. There is some evidence that in early diagnosed patients, anxiety can contribute to their ongoing symptoms [5] But this may be due to reading stories on social media making people more aware of possible symptoms.
However, some studies have found that a disrupted immune system may be the cause. These studies are few, usually with early diagnosed patients and use tests for immune system markers that are generally only available in a research setting. [6,7]
For a good overview of the problems involved in getting to the bottom of PTLDS see reference [4] below.
In the UK, a significant proportion of Lyme disease cases are diagnosed late [8]. See also our poster at the NordTick 2023 conference. We are pushing for a study to investigate late diagnosed patients as this may help to identify a potential cause, or causes.
What can someone do if they have continuing symptoms?
- Check with the NICE Guideline that you have had appropriate treatment, which is at least 21 days of antibiotics.
- If you still have symptoms, or new ones appear, talk to your GP, because NICE recommends a second course under certain circumstances.
- Talk to your GP about other possible causes of your symptoms.
- Keep a log of your symptoms.
- Discuss pain relief with your GP, and consider giving them a copy of this page so they understand the gap in science that you are coping with.
- Remember that many people continue to gradually get better – this might include you.
We shall update this information as more research is published that may help those with continuing symptoms.
References
- Concurrent Infection of the Human Brain with Multiple Borrelia Species. Golovchenko, Maryna, et al. 2023. International Journal of Molecular Sciences 24 (23): 16906.
- Lyme Disease in the U.K.: Clinical and Laboratory Features and Response to Treatment. Dillon, Richard et al. 2010 Clinical Medicine (London, England) 10 (5): 454–57.
- Characteristics and clinical outcomes after treatment of a national cohort of PCR-positive Lyme arthritis. Grillon A. et al. 2019 Semin Arthritis Rheum 2019; 48: 1105–1112.
- Persistent Symptoms After Lyme Disease: Clinical Characteristics, Predictors, and Classification. Baarsma ME, Hovius JW 2024. J Infect Dis 2024;230(Supplement_1):S62–9.
- Determinants of persistent symptoms after treatment for lyme borreliosis: A prospective observational cohort study. Vrijmoeth HD et al. 2023 eBioMedicine 2023;104825.
- Association of Persistent Symptoms after Lyme Neuroborreliosis and Increased Levels of Interferon-α in Blood. Hernandez SA et al. 2023 Emerg Infect Dis 2023; 29: 1091–1101.
- Elevated Levels of IL-23 in a Subset of Patients With Post-Lyme Disease Symptoms Following Erythema Migrans. Strle K et al. 2014 Clin Infect Dis 2014; 58: 372–80.
- Zoonoses reports England, NB data for 2025 onwards is not yet available.
- Clinical Course, Serologic Response, and Long-Term Outcome in Elderly Patients with Early Lyme Borreliosis. Boršič K, et al 2018 J Clin Med 2018, Vol 7, Page 506 2018; 7: 506.

 Printer Friendly
Printer Friendly