A Missed Opportunity?
For 15 years Lyme Disease Action (LDA) has been consistently advocating science, and robust evidence, in striving for the prevention and treatment of Lyme disease.
5 years ago LDA funded research with the James Lind Alliance (JLA) to establish the top 10 ‘unknowns’ about Lyme disease in the UK which need research. There were many more than 10 unknowns.
4 years ago LDA funded and co-authored the Royal College of General Practitioners (RCGP) e-learning module on Lyme disease.
On the basis of the government’s own conservative estimates, since LDA was founded there have been 45,000 new cases of Lyme disease. How many of these have been successfully treated is unknown. How many others remain un-diagnosed, or unsuccessfully treated, is also unknown.
Given what is known about the lack of evidence on which to base diagnostic and treatment decisions, LDA had mixed feelings about the 2015 decision of the National Institute for Care and Clinical Excellence (NICE) to produce a National Guideline on the diagnosis and management of Lyme disease. However, LDA engaged in development of the scope and Guideline, with its chair selected to the committee as a lay member, and commented in brief on the Draft when it was released for consultation in September 2017.
Amongst the potential gains LDA anticipated & hoped for were:
- strides forward in health professionals’ awareness particularly in critical early treatment;
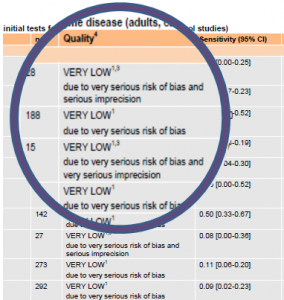
- an acknowledgement of the known uncertainties and poor quality of evidence available;
- provision of specialised clinics and a raft of research recommendations.
While acknowledging the guideline is still in draft, and may yet change, LDA is concerned that these potential gains may be unrealised.
 Therefore LDA’s detailed response on the draft guideline, published here, has an overall tone of disappointment. In real terms, the gains right now are small, but there is hope it will help improve the recognition, diagnosis and treatment of early Lyme disease. The position of patients, and clinicians supporting them, is not greatly advanced over that represented by the 2015 revision of the NICE Clinical Knowledge Summary (CKS). Both these currently have, as the safety net for patients, “refer to a specialist”. It is bitterly disappointing, then, to not have strong recommendations on the establishment of specialist clinics for Lyme disease, which LDA has been vigorously advocating, to develop specialist clinical expertise and conduct much needed research.
Therefore LDA’s detailed response on the draft guideline, published here, has an overall tone of disappointment. In real terms, the gains right now are small, but there is hope it will help improve the recognition, diagnosis and treatment of early Lyme disease. The position of patients, and clinicians supporting them, is not greatly advanced over that represented by the 2015 revision of the NICE Clinical Knowledge Summary (CKS). Both these currently have, as the safety net for patients, “refer to a specialist”. It is bitterly disappointing, then, to not have strong recommendations on the establishment of specialist clinics for Lyme disease, which LDA has been vigorously advocating, to develop specialist clinical expertise and conduct much needed research.
The final guideline will not be mandatory, but since NICE guidelines are generally used as a quality standard, there will be an expectation that clinicians should not usually deviate from NICE recommendations without clear justification. This does leave clinicians free to continue using their clinical judgement (as at present), but they will need to be able to adequately defend any clinical decisions that are outside the recommendations. However, hard pressed GPs are likely to simply look at the tables detailing antibiotic choice, dose and duration and apply them, unaware that the recommendations are based mainly on current practice. In the accompanying appendices the evidence base on efficacy is acknowledged to be poor. Will any health professional have time to read these? It seems likely that “clinical judgement” will, in practice, remain uninformed by this important caveat.
We wait to see how the Guideline Committee respond to the stakeholder comments they receive.

 Printer Friendly
Printer Friendly